Something had happened. The hospital lies on the main stretch of road before the town of Borgne, right across from the high school, so there is always a lot of activity going on: cars going in and out of the hospital, motorbikes dropping off and picking up students, vendors selling food and cell phone credit. But this was different. The cries were not those typical of school-aged children. Plus, it was already 8 p.m., way past the time the last student had left.
Something had happened. The hospital lies on the main stretch of road before the town of Borgne, right across from the high school, so there is always a lot of activity going on: cars going in and out of the hospital, motorbikes dropping off and picking up students, vendors selling food and cell phone credit. But this was different. The cries were not those typical of school-aged children. Plus, it was already 8 p.m., way past the time the last student had left.
A few days prior, water and sanitation teams had been uncharacteristically meeting late into the night discussing who knows what. I am new to the hospital compound, so I don’t always feel comfortable snooping around asking everyone what is going on. But tonight, the wailing was eerily familiar. A 35-year-old woman had just died from cholera.
Ever since the epidemic began on Oct. 13, 2010, nine months after the earthquake, managing this archaic, yet vicious disease has been a massive undertaking, especially given the debilitated-at-best state of public health infrastructure, water and sanitation. Despite these challenges, the epidemic has been controlled reasonably well by the hospital here, keeping cases to a rare few in the dry season and a half-dozen during the rainy season. Despite the incredible efforts carried out by Alliance Sante Borgne (ASB)—the H.O.P.E.- and Ministry of Health-managed hospital in Borgne—this woman was unable to seek care in time for dehydration to take its toll. Everyone in the compound is visibly distressed. Many take the death as a personal failure.
I have been in Borgne for two weeks now. My days consist of shadowing physicians in a variety of contexts in the morning, while my afternoons are spent relishing the task of converting the hospital records to an electronic system: an endeavor frustrating enough in an industrialized country, verging on insane in a place like this. There are a few other foreigners, helping to work on the transition to e-records in addition to carrying out a pilot study for a potential project tackling heart disease.
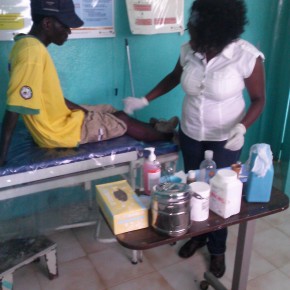
The clinic ranges from a traditional hospital setting to a child malnutrition ward, hosting (or providing) prenatal visits, general consults, emergency intake and even a rural clinic a few hours away by foot. As expected, I feel a bit useless snooping around and asking questions in my clumsy Creole, but the attending physicians are incredibly professional and never protest a request by me to shadow. Most have been trained in Cuba at the prestigious Escuela Latinoamericana de Medicina (ELAM). The ELAM offers scholarships to qualified applicants from countries that lack the capacity to train physicians from poor communities, including a small group of American medical students from under-resourced communities. The program began taking Haitian students on about 10 years ago and has had a massive impact on health care access for the population. It has been said than when Thony Voltaire, the young ASB medical director, came back to his hometown as a new physician, he had people lining up to see him. For weeks he carried out consults without rest. Now the hospital staffs seven physicians, five trained in Cuba and two in Haiti.
As a medical student, the clinical exposure I am receiving is at times unbelievable. I remember just finishing our unit at Rochester this past spring on parasitology and students bewildered at the seemingly endless stream of parasites most had never heard of. Some asked why we had to learn about topics never seen in the United States. Similar questions were raised when learning about tuberculosis and cholera.
On my fourth day in Borgne, I was able to visit one of the rural clinics and followed one of the family physicians doing consults. A young woman and small child came in next. One sentence came out of the mother’s mouth. The physician turns to me and says, “TB.” I couldn’t believe it. The child looked thin, but nothing more dramatic than anyone else I had seen. Then I listened to his lungs and it sounded like crushing tin foil. After a few more questions the child started coughing and the mother’s small tissue couldn’t manage to capture all the blood that came out. I was floored.
You can read all you want about how devastating a disease like tuberculosis can be, but there is a moment when it switches to something real and powerful and terrible and unfair. I have seen two more cases since then and among the next two, the levels of wasting were much more dramatic. The hospital provides the drugs free of charge, but there are so many extraneous factors that prevent individuals and their families from accessing care. The commune of Borgne is vast and mountainous. It can take hours, and in some cases days to reach a hospital. Small, rural living quarters exacerbate the spread of this airborne pathogen. Observed treatment can be difficult to organize.
For those of you familiar with the history of poverty and health care in Latin America and the developing world, some of this may not be surprising. There are a handful of organizations doing spectacular work managing unmanageable health care issues. Nevertheless, the problem is deeper than that which can be solved by charitable organizations. This of course is not to say that the impact of hospitals such as ASB is anything less than extraordinary. This is a fact to which every individual touched by this hospital will attest. It does, however, beg the question of what will happen to communities of the same size that have little more than an empty room and a transient nurse as their local hospital. Indeed this was what the health system of Borgne looked like 15 years ago.
As future physicians, it is impossible not to ask the questions necessary to heal our patients clinically. When poverty and economic injustice create the conditions necessary for treatable diseases such as cholera and tuberculosis to mercilessly take the lives of our patients, we should maintain our responsibility to ask questions, even if the answers are economic or political.
This is important for those of us who believe health is a human right in any place, but it is also important for improving health care in our own country and, at the most cynical level, to prevent the emergence of pathogens that pay little respect to international borders.
As for me, I will try to remain a fly on the wall and check back soon.
Haiti Teaches is a column that explores the opportunities, nuances and conflicts associated with time spent as a medical student in a foreign country. It follows a second-year medical student before, during and after his two months with a community development organization in Borgne, Haiti.