Yash Shah (5 Posts)
Yash Shah (5 Posts)Columnist and Medical Student Editor
Sidney Kimmel Medical College at Thomas Jefferson University
Yash attends Sidney Kimmel Medical College at Thomas Jefferson University in Philadelphia, PA. He pursued a Bachelor of Science in premedicine at Penn State University. Prior to attending medical school, Yash worked on clinical and translational oncology research at the Children's Hospital of Philadelphia. He has long-standing interests in contributing to medical education, advancing health policy, and working with cancer patients. He enjoys playing tennis, rooting for the Eagles, reading, and traveling in his free time.
COVID Chronicles
The COVID-19 pandemic posed a tremendous challenge to our community – certainly from a health perspective, but also in nearly every other aspect of daily lives. Our daily routines were upended – from the way we work, play, learn, socialize and travel. Numerous times, the unimaginable happened, and it is safe to say we will never see the world in the same way again. As future physicians, it is important that we recognize the challenges faced by the health care space during the pandemic, and perhaps more importantly, the everlasting transformations that our future medical students, physicians and patients will encounter. This column explores the countless obstacles we overcame and their everlasting effects, along with emerging trends that we will see in health care for the years to come.
The COVID-19 pandemic and its associated lockdown precipitated wide-ranging effects on nearly all aspects of our society. Perhaps some of the most severely affected patients were those fighting cancer. These patients have little physiologic resistance to COVID-19 and accordingly experience higher morbidity and mortality when infected.
Students across the country in all grade levels, from preschool to graduate school, had their educational routines upended by the COVID-19 pandemic and its associated lockdown. In medicine, there were special challenges associated with adapting safety protocols to a field that inherently requires human interaction.
Mr. T did not smile at me. No, I didn’t think it was because he was mean or anything; in fact, he was polite and had quite a calming voice. But honestly, it was hard to read someone’s facial expression behind a mask — at least during the first few months of the COVID-19 outbreak.
As COVID-19 continues to rage around the world, extended quarantine measures have been responsible for saving innumerable lives. Now, as we slowly catch glimpses of light at the end of the tunnel, or face the possibility of rising cases returning us to the heights of the pandemic, it is important to examine the long-term side effects of our self-prescribed quarantine treatment.
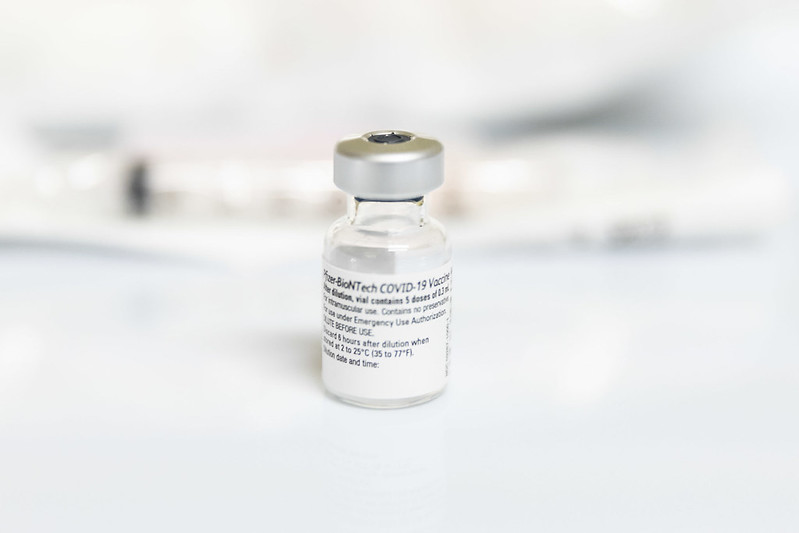
With the development and distribution of the COVID-19 vaccine and the arrival of the summer season, people are feeling happier and beginning to come out of their homes. It’s clear that there is a growing sense of hope that the pandemic may be approaching its conclusion. However, standing in the way of our pursuit of normalcy is the refusal among some to partake in the vaccine, despite its proven efficacy and safety by experts.
None of us pictured beginning medical school in a pandemic. Most of us are still in shock we were admitted to medical school owing to severe imposter syndrome. Despite the exceedingly virtual nature of the fall semester — as of now, our only in-person activities are optional anatomy labs — we have hitherto made the most of this experience. Undeterred by the inability to partake in many in-person activities as a class, we are fostering meaningful relationships with our peers online and in person.
Rather than ask elderly poll workers to risk their health on Election Day, medical professionals and students can volunteer to work at polling locations. Health care professionals and students tend to be in a lower-risk population and are also well-versed in the public health practices critical to safely conducting an election during the pandemic.
How could I study for my next exam instead of focusing my energy on the crisis around me? Was I selfish for still worrying about doing well in school while others died alone in the hospital on a ventilator? In these moments, I found respite in “Learning in War-Time,” a sermon delivered by C.S. Lewis to the students of Oxford in 1939 just as World War II began. In this timely sermon, Lewis addressed the chief concern on students’ minds: Why continue to study philosophy or science “when the lives of our friends and the liberties of Europe are in the balance?”
I am worried that these stories of heroism are harming the very people they celebrate. By creating an ideal “health care worker” as an endlessly altruistic individual, it stigmatizes the medical workers who refuse to take on these risks — even though there are many legitimate reasons not to.
Yes, unfortunately, I have become one of the 60,000 and rising daily cases in the nation. Yet, I am one of the lucky ones.
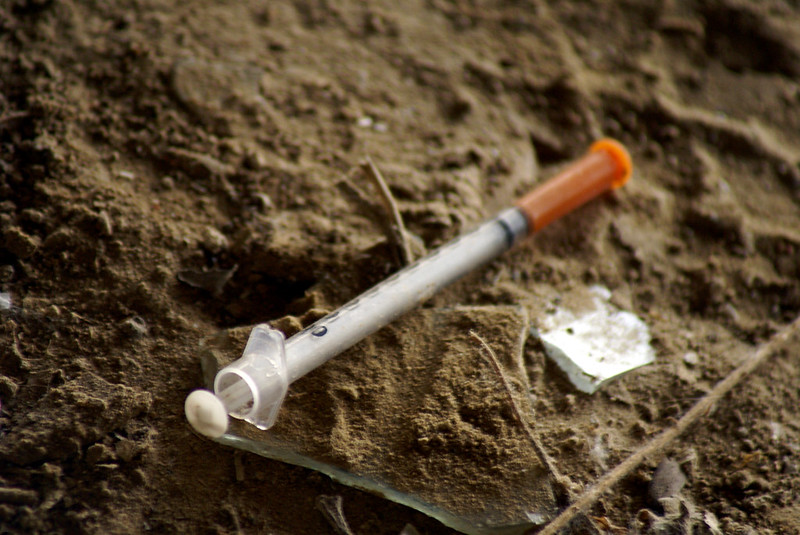
For a variety of reasons, the substance use population is particularly vulnerable to the impacts of the COVID-19 pandemic. Based on data from previous financial crises, the emotional toll will increase rates of new substance use, escalate current use, and trigger relapse even among those with long-term abstinence. There may be a significant lag before these changes are detected and treated because health care resources are being funneled toward the pandemic.
Never committed a crime, / but now I feel like a prisoner. / Trapped in our minds, / our spirits leashed, / our existence wanders among these all too familiar walls.
 Puja Mohan (2 Posts)
Puja Mohan (2 Posts)Contributing Writer
Northeast Ohio Medical University
Puja Mohan is a second year medical student at Northeast Ohio Medical University. In 2019, she graduated from Kent State University's BS/MD program with a Bachelor of Science degree. In her free time, Puja enjoys writing, music, as well as spending time with friends and family.