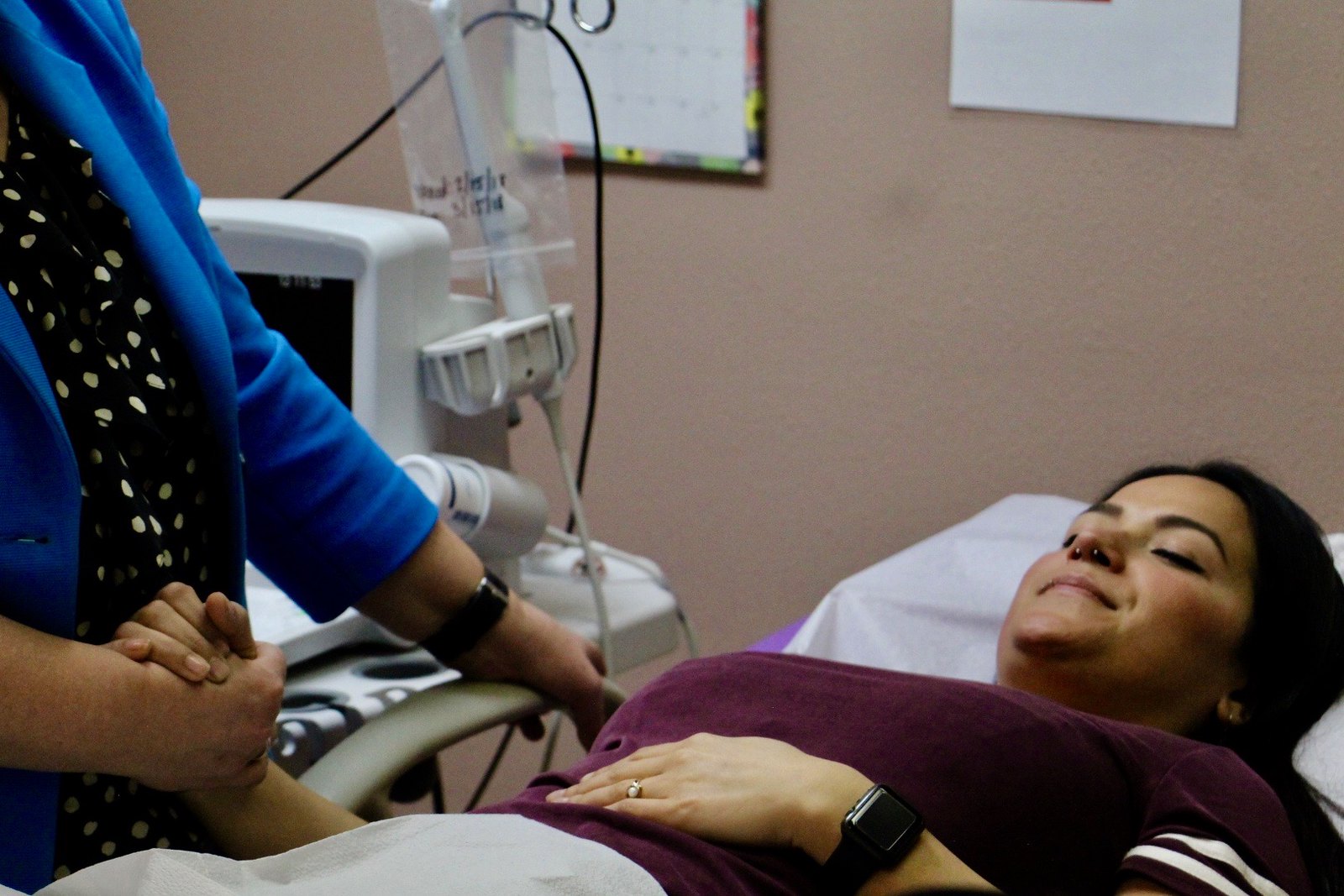
Cancer Care Among Health Care Students: A Key Towards Building a Sustainable Cancer Care System in Rwanda
When I was a child, I lost my grandpa to cancer. I used to promise him that I would become a health care provider and heal him, but unfortunately he passed away when I was in twelfth grade. Later, I joined medical school at the University of Rwanda, where I became involved in student-led research, health promotion practices and knowledge measurement.