“Telestroke,” a telemedicine approach to acute stroke care, is revolutionizing how we treat our country’s third leading cause of death. Leveraging modern communication technology and the combined experience of skilled neurologists, Telestroke aims to benefit patients in rural areas who are often at the highest risk of ischemic stroke but have the least access to treatment. In many ways, Telestroke allows patients, no matter where they are, to receive expert care for a condition that requires timely intervention and is a shining example of telemedicine in action.
By the World Health Organization’s definition, telemedicine (also called telehealth) is “the delivery of health care services … using information and communication technologies for the … diagnosis, treatment and prevention of disease.” In his 1974 article, “Telemedicine: The Missing Link Between Homes and Hospitals,” Roger Mark dreamt of a way for physicians to keep up with their patients remotely, without requiring their physical presence at a hospital. What once seemed like science fiction is now a reality, and it is emerging as the standard of care. Telemedicine has found a home in practically every medical specialty and has attracted attention from both investors and critics. In 2014, on-demand health care companies saw a 300% increase in year-over-year funding, propelling companies like Teladoc, a service that provides on-demand medical care via mobile devices, into the top five funded on-demand companies alongside the likes of Uber and GrubHub.
Many telemedicine systems operate on a “hub and spoke” model. A single “hub,” like a large urban hospital, serves numerous “spokes,” which could be rural clinics, under-staffed hospitals or even a patient with a smartphone. In the Telestroke model, the hubs are comprehensive stroke centers and the spokes are clinics without experts in acute stroke treatment, often in rural areas. This allows stroke experts to eliminate the obstacle of distance in most cases and remotely direct treatment of patients with stroke symptoms.
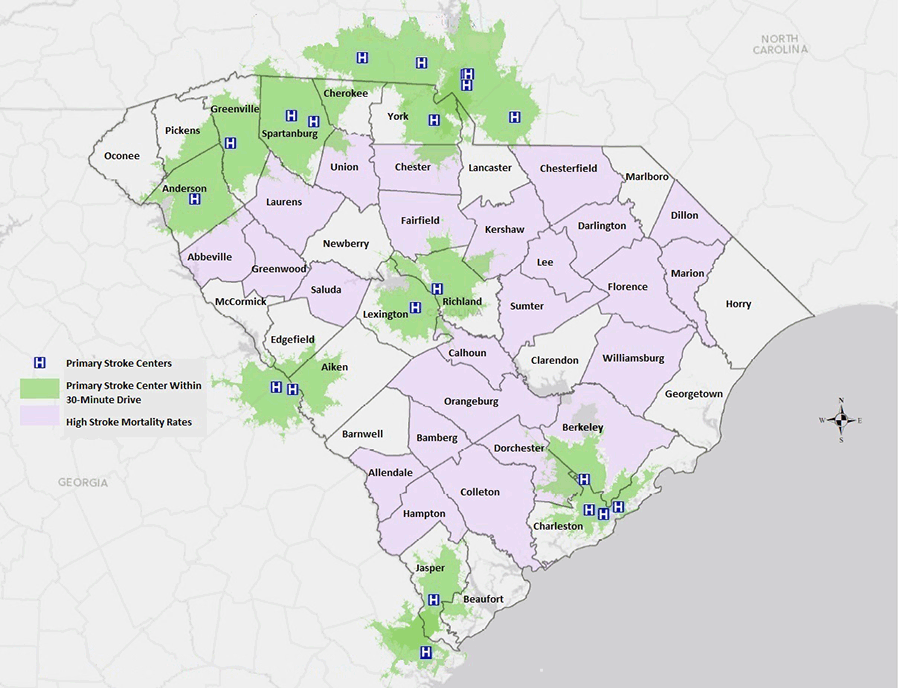
Figure 1. Patients in South Carolina who are located more than 30-minutes from a comprehensive stroke center are at a higher risk of mortality due to a stroke. See Figure 2 for a look at how Telestroke programs aim to improve outcomes (Samson et al., 2015).
This “hub and spoke” model has proven to be particularly promising in the management of ischemic stroke patients. “Time is brain,” neurologists like to say, as treatment must be administered within six hours of onset in order to avoid long-term complications. Unfortunately, rural clinics often do not have access to the same battery of treatment options as primary stroke centers or are hesitant to use them due to lack of experience or potential complications. For this reason, patients are often transported by helicopter to the nearest comprehensive stroke center, wasting precious time and resources. Neurologists are using Telestroke to bridge this gap by acting as consultants on Telestroke platforms, using their expertise to guide on-site physicians through a patient’s treatment with drastically improved outcomes. Patients treated via Telestroke hubs have significantly longer long-term survival than those treated by spoke physicians alone, with in-hospital mortality on par with that of patients treated on-site at comprehensive stroke centers.
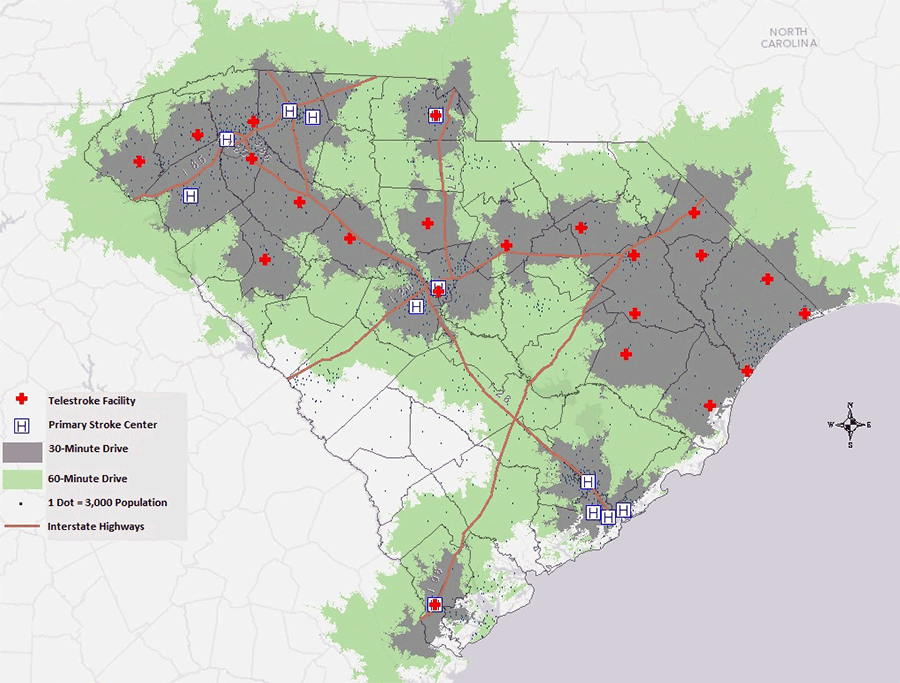
Figure 2. Telestroke Hubs in South Carolina are strategically established to increase access to stroke care. Individual dots can be thought of as “spokes” that can be served remotely by (or transported to) nearby hubs. It is estimated that after the establishment of these hubs, over 95% of the state’s population can receive expert stroke care from within an hour of where they live (Samson et al., 2015).
Telehealth programs like Telestroke have clearly demonstrated their value in the modern health care system, so why aren’t they more pervasive? Ostensibly, telemedicine is a win-win-win for patients, providers and payers. Despite its obvious merits, a few key barriers stand in the way of telehealth becoming the Facebook of doctor’s appointments. First, and perhaps most challenging, is physician licensure and credentialing. The implementation of telemedicine is complicated by the fact that physicians may only practice in states in which they are licensed. While there are a limited number of states that offer cross-state licensing for these purposes, the majority of physicians are forced to practice within a state or pursue additional licensure. Pushback from individual states that are unwilling to give up revenue garnered by issuing licenses means that this paradigm is unlikely to change anytime soon. Second, a barrier has arisen in the form of Medicare reimbursement policies and private payer coverage. Most states do not reimburse telemedicine consults unless the patients are located in a “non-metro area” (read: rural), discouraging the use of telehealth for follow-ups or monitoring of local patients. In fact, most states do not even require private insurance providers to cover telehealth services at all. These obstacles evidently stem from the complex interplay between state and federal health care policy and, while delving into this rabbit hole might be the subject for another article, it is clear that a policy overhaul would be necessary to get telemedicine into the average household. However, in those states in which telemedicine laws are more relaxed, we’ve seen it flourish in some interesting (but not unexpected) forms. For instance, several California-based companies have adopted a telemedicine approach to connecting patients with physicians who can write them a prescription for medical marijuana.
Despite the administrative nightmare it presents, telemedicine actually solves more problems than it creates. Telemedicine will undoubtedly play a role in our future medical practices and will hopefully provide a more rewarding experience for both our patients and us as providers. It allows the rising tide of biomedical research to truly lift all boats. Innovative medical practices and technology that reach a telemedicine hub provide instant benefit to all its spokes, ensuring a uniform standard of care. The future of telemedicine is uncertain but will likely see a rise in “direct-to-consumer” services like Teladoc, foregoing the role of physicians as consultants on telehealth platforms and allowing them to take better control of their patients’ care. Truly disruptive innovation tends to encounter seemingly insurmountable barriers, and telemedicine is no different. The widespread success of this technology to date provides us with an exciting glimpse into the future of our field and is proof of that the discomfort of changing the way we do things might just be worth it.

