“You Must Hate Patients”
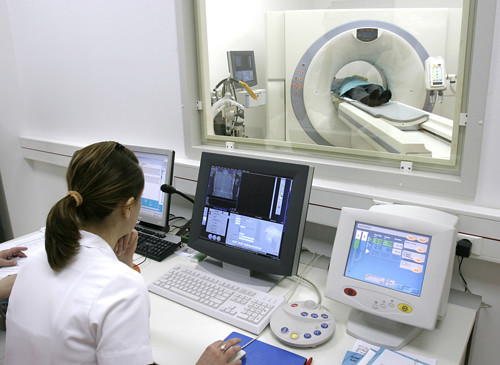
From premed onward, an interest in pathology is often met with a well-meaning but mildly disapproving joke. It comes from friends, family, mentors and internet forums. “You must hate patients.” It seems introverts and misanthropes alike are often relegated to the sub-sub-basements and windowless corners of the hospital, where radiologists and pathologists hiss at lost patients. While every specialty is ripe with ridicule and stereotypes, this particular joke damages the image of an already underappreciated …