A patient in the intensive care unit (ICU) suddenly develops respiratory distress and hypoxemia. Her lungs sound clear bilaterally. She is placed on supplemental oxygen via face-mask while a chest angiography is ordered to assess the possibility of a pulmonary embolism. Unfortunately, the patient’s oxygen saturation drops further. The nurses want to know what the next appropriate intervention is. But you can’t answer. You are tongue-tied. You shift your gaze nervously…
Relax. This is a simulation planned by your medical school to teach emergent cardiorespiratory support as part of your pulmonary physiology course. No one’s life is in danger. Furthermore, unless you have read far ahead, you should not know the answer to the nurses’ question yet, especially since you are a long way from caring for patients in an ICU.
The modern medical school simulation uses an integrated approach to place the information learned in class within the wider clinical context. Simulations can be further classified as human simulators (mannequins that mimic physiological states), task trainers (standard mannequins/tools), humans (standardized patients) or virtual reality platforms. In the curriculum, simulators are used for both instruction and assessment.
The first simulators for medical training were Resusci-Anne, designed in 1960 to teach CPR, and the ever-beloved Harvey, designed in 1968 by the University of Miami to teach cardiac murmurs. In line with their original uses, simulators are still frequently used to teach Basic Life Support, Advanced Cardiac Life Support and Pediatric Advanced Life Support.
There have also been advances. For example, nowadays, simulations have gone as far as using virtual reality (VR) technology. A few exciting VR innovations include:
- An anatomy course by Unimersiv done with a Samsung VR headset and without the use of a cadaver
- “We Are Alfred”: an immersive system by Embodied Labs that allows students to develop empathy for elderly patients by having them experience the audiovisual problems these patients experience
- Trauma room simulations by the Royal College of Surgeons in Ireland
- “The Virtual Surgeon”: a 360° operating room experience by Medical Realities
Simulations are integral to the curriculum for a few reasons. Foremost, they are excellent teaching aids; indeed, this is why the Association of Standardized Patient Educators has provided standardized patients for the USMLE Step II CS since 2005. They help students hone their craft in a low-risk setting. In the above example, when you became tongue-tied while your patient’s oxygen saturation drops, no one was harmed at the expense of your learning. Simulations also offer the convenience of being able to manipulate the simulators to portray scenarios that align with the student’s coursework and skill level. This provides more targeted learning, which is not always possible in real and complex patients. Additionally, simulations often involve students from different schools and different programs, which helps students enhance their interdisciplinary communication as well as understand the tasks and skills of other health care professionals. Finally, simulations offer the opportunity to receive real-time constructive feedback from one’s preceptor and simulator. Standardized patients have the added advantage of assessing one’s interpersonal skills and professionalism.
Simulations are also a way to provide exposure for students. For example, simulators can teach the clinical skills for which a student may not have ready access to real patients, such as performing pelvic exams. These types of physical exam skills are vital to learn prior to performing them on real patients, given their invasive nature. Additionally, simulators are able to portray the gamut of ages and disease stages that students might otherwise not see on the wards.
It should be noted that knowledge and skills rarely become memorable after a one-time simulation. This is why simulation centers in medical schools, which are accredited by the Society for Simulation in Healthcare, allow students unfettered access to repeatedly practice skills on their own time and integrate their own learning into their simulation experience.
The use of simulations also provides a better understanding about some of the clinical skills used in multiple residencies, most notably surgical specialties and emergency medicine. Many of the skills used in these fields that intimidate medical students, such as placing central lines via ultrasound guidance, are now being routinely taught in medical schools by residents and attendings. Subsequently, medical students are more comfortable with the work of various specialties as they start assessing potential choices for residency.
Several studies have demonstrated the effectiveness of medical school simulations. Chakravarthy et al. showed that simulations help with retention of basic science lessons while Aboumatar et al. and Bearman showed that simulations help students develop communication, safety skills, and empathy. Furthermore, going beyond medical school, Vadnais et al. showed that the ability of physicians to use a skill was related to the degree of short-term confidence they gained after undergoing a simulation for that skill.
While simulations have many benefits, they do have their limitations, especially when used within the first two years of medical school. Firstly, even though the setting is low-risk, it is quite daunting to perform a skill while one is still trying to grasp its theoretical underpinnings and remember all its steps; this contributes largely to the hesitance I have seen among medical students during simulations. Fortunately, this improves after one has experienced a few simulation sessions. Secondly, the skills taught in simulations, such as administering CPR correctly, are best remembered through repeated practice — practice which is cemented by clinical exposure. Since the first two years of medical school are classroom-based, students may see or perform these skills during only one simulation session. While some students do have free access to their school’s simulation centers, unless one is enthusiastic about the skill and dedicates time to practice it, the deluge of coursework may easily assume a greater priority.
Fortunately, both of these limitations can be remedied by integrating more simulations into the curriculum! For this reason and due to the many benefits of simulation enumerated above, the use of simulators should continue to play a central role in medical school education.
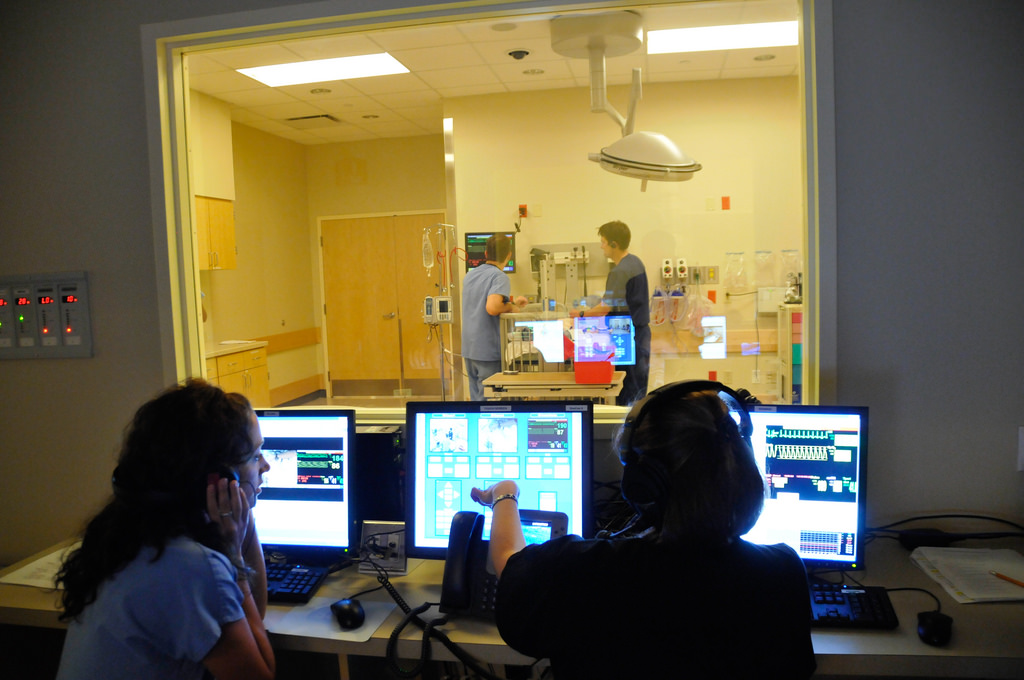
Image credit: “The Simulation Center” (CC BY-NC-ND 2.0) by IU School of Medicine