Allison Chin (1 Posts)
Allison Chin (1 Posts)Contributing Writer
Florida International University Herbert Wertheim College of Medicine
Allison Chin is a fourth-year medical student at Florida International University Herbert Wertheim College of Medicine in Miami, FL in the class of 2023. In 2017, she graduated from the University of Miami with a Bachelor of Science in biochemistry and nutrition, along with minors in chemistry, psychology and art. She was inducted in the Arnold P. Gold Humanism Society and awarded the President Volunteer Service Award and the Florida Board of Medicine Medical Student Recognition Award in 2022. She enjoys custom card making, yoga, painting, and discovering new red wines and dark chocolate in her free time. After graduating medical school, Allison would like to pursue a career in Internal Medicine.
During the last week of my clinical rotation in family medicine, my attending advised me and the accompanying medical student that going forward, the health providers of the clinic must limit their scope of care for patients who present for annual examinations.
On May 2, POLITICO published the leaked SCOTUS majority opinion draft indicating the imminent intention of the court to overturn Roe v. Wade, Planned Parenthood v. Casey and 50 years of legal precedent that ensured access to necessary health care for anyone capable of becoming pregnant.
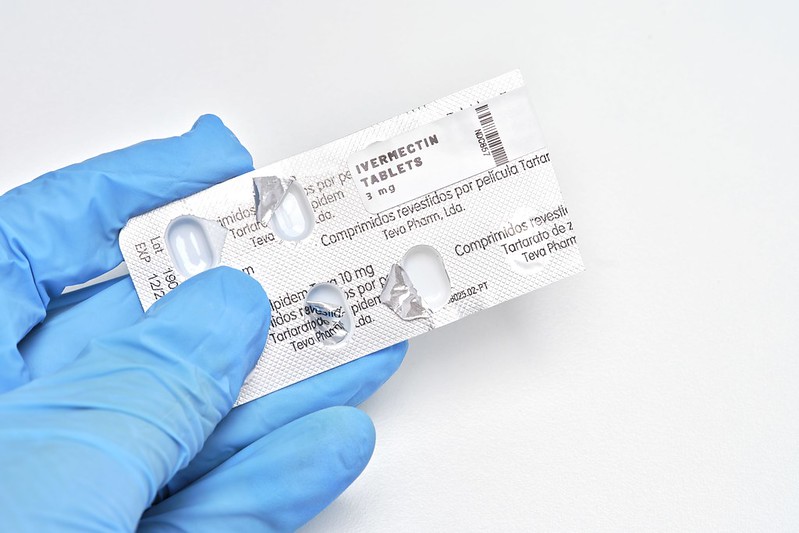
Like many medical students, I am familiar with the antiparasitic medication ivermectin, a common drug taught in medical school. Ivermectin became an unexpected subject in the COVID-19 pandemic. However, after seeing a patient in the clinic taking ivermectin as an alternative to vaccination, the news hit differently.
The COVID-19 pandemic’s devastating effects upon our nursing homes has highlighted the vulnerabilities of this sector of our health system. With increased attention to the issues in such a growing and vital part of our society, we have a once-in-a-lifetime opportunity for change.
In today’s landscape of rapid innovation, medical providers need to quickly adapt in order to thrive in an ever-changing field. Better yet, we need to be equipped to lead and guide the innovations so that we are not just “reactors” to change, but rather the drivers of progress in health care.
Many women have experience with using or trying to attain access to contraceptives. More than 100 countries offer contraception over the counter; however, the United States is not one them.
An anxious, 36-year-old Hispanic female lays on the exam table, her feet in stirrups. A sleeved arm juts out between her tented legs as she stares resolutely at the ceiling. I wonder if she is afraid of what the amorphous black and white structures shifting on the ultrasound monitor may reveal.
Many in our nation see COVID-driven requirements as anathema to their independence, but what if mandates are actually the best way to secure our personal liberties?
The idea of prescribing housing sounds too good to be true, the exact kind of thing you would expect to see on a medical drama. It couldn’t possibly work in real life … or could it?
In this episode we interview Dr. Ijeoma Nnodim Opara. Dr. Opara received her medical degree from Wayne State University School of Medicine (WSUSOM) and completed a med-peds residency at the Detroit Medical Center where she served as chief medical resident. Currently, she is a double-board certified and an assistant professor of internal medicine and pediatrics.
In 2018, a patient filed a complaint against a medical student for wearing a “Black Lives Matter” pin on her white coat. When the student reached out to her school’s administration, she received this response: “It is best to not raise barriers in the way we present ourselves … Some of your political pins may offend some people, and it is probably best not to wear them on your white coat or while you are working in a professional role.”
The notion that a person’s health is only impacted by the clinical care they receive is not a reasonable one. Currently, as a first-year medical student, I have had the privilege to learn from a variety of professionals that have once again reminded me why I am on this path and why I want to serve underserved populations.
 Alma Esparza Castañeda (1 Posts)
Alma Esparza Castañeda (1 Posts)Contributing Writer
University of California Riverside, School of Medicine
Alma is a second-year medical student at the University of California Riverside, School of Medicine in Riverside, California class of 2023. In 2015, she graduated from the University of California, San Diego with a Bachelor of Science in human biology. She enjoys playing soccer, board games, and spending time with family and friends in her free time. After graduating medical school, Alma would like to pursue a career in pediatrics.