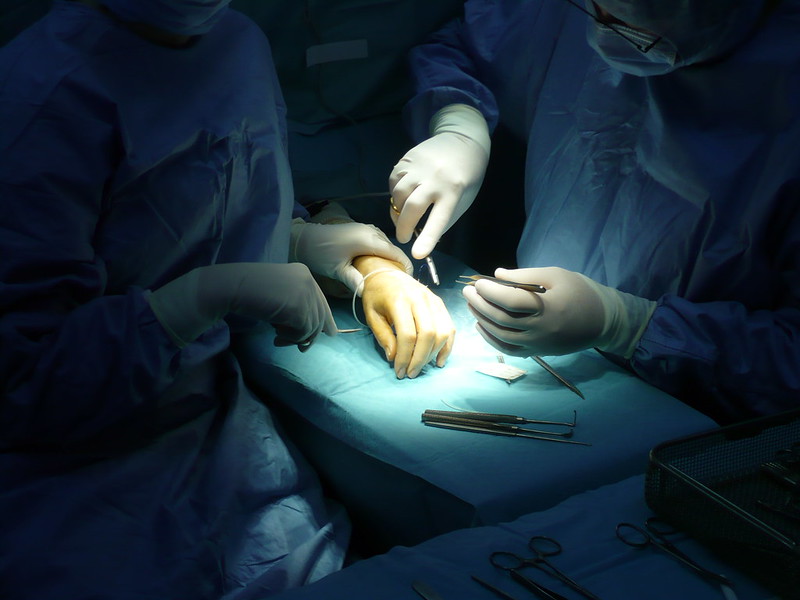
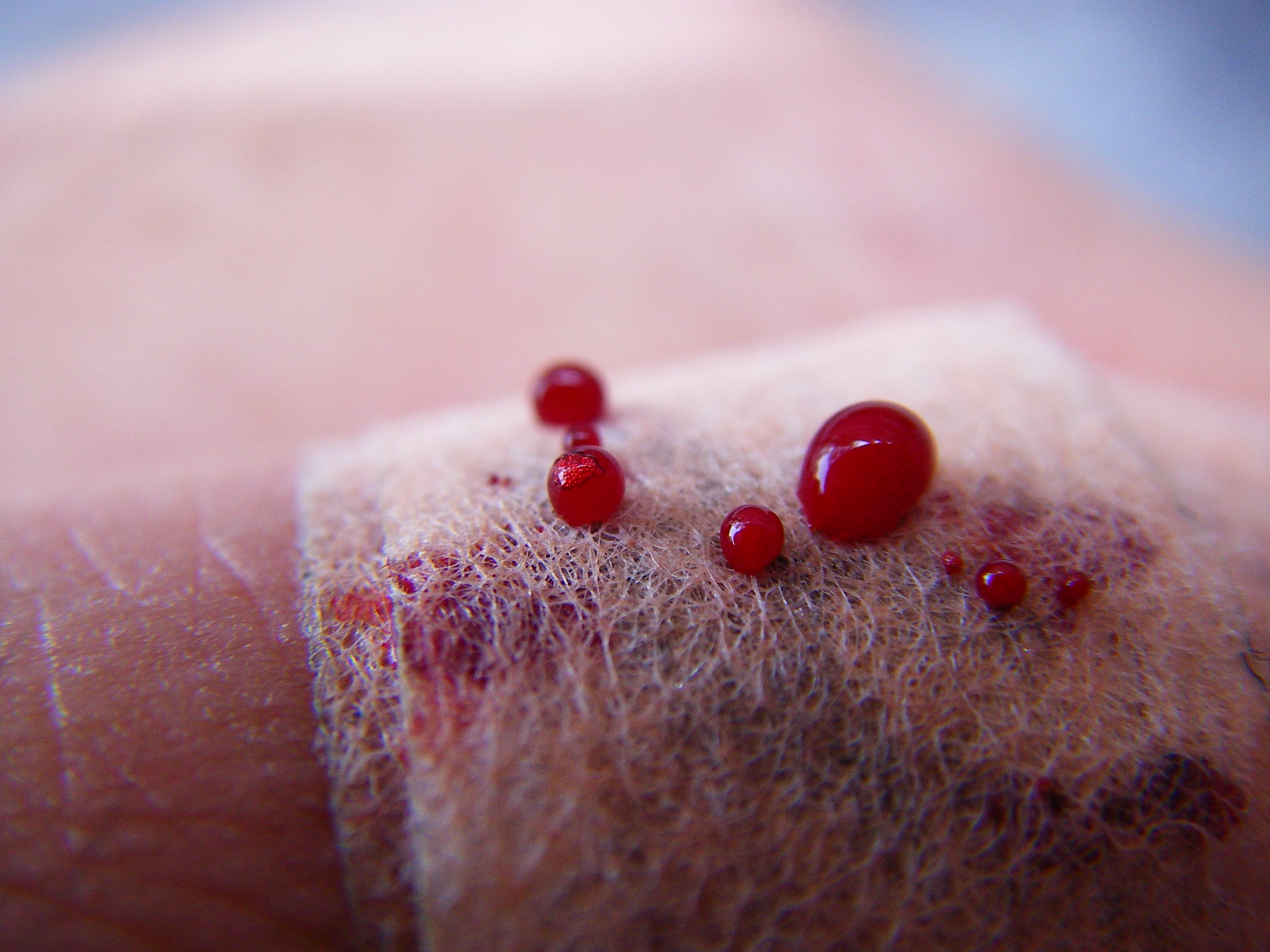
Finding Balance in the Wake of My First Code Stroke
As we got closer to the ED, the excitement evolved into a feeling of discomfort. It was uncomfortable to feel even briefly excited by another person’s misfortune. I felt a sense of disequilibrium as I realized I had strayed from the delicate balance medical students and physicians continually try to find.