Kaitlin Toal (3 Posts)
Kaitlin Toal (3 Posts)Writers-in-Training Intern and Contributing Writer
Geisinger College of Health Sciences
Kaitlin is a medical student at Geisinger College of Health Sciences, class of 2027, interested in primary care and addiction medicine. She is from Malvern, PA and attended Northeastern University for undergrad. Outside of school, Kaitlin loves running, volunteering, cooking, reading/writing, and playing piano!
“254?!” I gawk at the glucometer, stunned that Tom’s blood sugar has soared to such heights when it has consistently remained below 125 for the last two weeks. Tom glances up at me with an amused look on his face, clearly entertained by my reaction — “It was probably that pork chop that did it.”
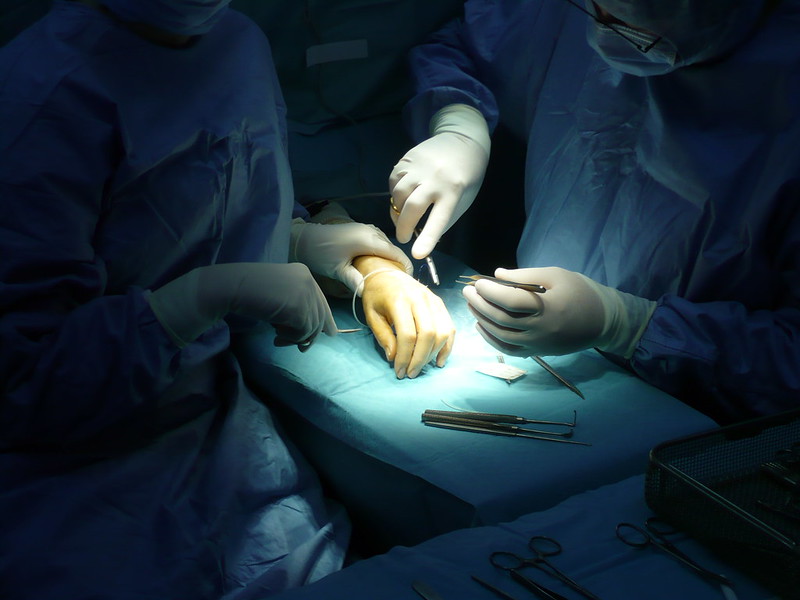
My first time in the operating room (OR) was when I was a junior in college. I was beaming under my mask, so excited to shadow and observe my first surgery ever, a riveting and exotic procedure: a planned and standard laparoscopic cholecystectomy. A friendly circulating nurse that I had been chatting with asked me, “Sabrina, what’s your glove size?”
After spending nearly a lifetime as a Type A perfectionist who struggled with developing new skills, I had spent the last several years trying to adopt a policy of “practice makes progress.” I have learned to accept the fact that being bad at something is often the first step towards being good at it.
Skepticism of health care is widespread throughout some of these communities — rightly so due to historical mistreatment, discrimination and lack of representation along with cultural differences. This distrust may be further strengthened by a patient’s own personal experiences. I respected this wariness, but I had yet to witness it firsthand.
In order to honor these works as well as celebrate the start of the New Year, we asked each of our editors to share their ‘Editors’ Pick,’ a must-read piece from 2023 that showcases the talent and breadth of our contributors.
Within the first week, the excitement I felt at my white coat ceremony quickly faded as I became overwhelmed and fell behind. Even with seemingly endless hours of studying, I was still doing poorly. I was exhausted every day and neglecting my well-being. For the first time in my life, my hard work was not paying off.
Throughout the COVID-19 pandemic, I kept myself sane by writing “Notes from the 13th Floor” — a series of moments I wished I could share with the outside world and the kind I never wanted to forget.
The stress of juggling multiple projects, some of which held little interest, seemed to overshadow their summer which should have been devoted to personal and professional development. In addition, I began to question if some of them would attempt to take shortcuts in their research.
The illness experience is chiseled by the search for meaning, for purpose, for greater understanding of existential suffering. This search is at the center of the spiritual journey.
A physician’s two favorite words: diet and exercise. Patients are constantly told that lifestyle interventions are the most important modifiable risk factors to prevent chronic illnesses like diabetes and hypertension.
In light of obesity’s concerning prevalence and economic burden, it becomes imperative that we equip future health care providers with the knowledge and skills essential for effective obesity management. However, despite the numerous consequences of obesity on both individuals and society, medical students are often found to be inadequately prepared to discuss weight management with patients.
Despite ongoing efforts and changing perspectives, gender equity in surgical specialties has not yet been achieved and is not simply a problem of the past. Only in addressing deep-seated gender roles and actively creating opportunities for the representation of women and gender-diverse persons in surgery can surgeons in Canada accurately reflect the populations they serve.
 Isis Lunsky (1 Posts)
Isis Lunsky (1 Posts)Contributing Writer
Queen's University
Isis Lunsky is a medical student at Queen's University in Kingston, Ontario, Canada, Class of 2024. Prior to medical school, she graduated with her bachelors in health sciences with a minor in chemistry from Mcmaster University, in Hamilton, ON. In her spare time, she loves reading, baking scones, choreographing dance routines, and supporting local theatre. After medical school, she hopes to pursue a surgical career where she can advocate for equity in the field as well as within medical education.